It’s Monday morning, the alarm is going off and the last thing you want to be doing is getting up and going to work. If you’re like me then you have a love-hate relationship with mornings. As soon as I’m up mornings are the most productive part of my day, but that first step can be a struggle. For some people that first step is not just the difficulty of getting out of a warm bed, but first step pain (known as post static dyskinesia) particularly in the heel, is an incredibly common and painful symptom for many people.
Heel pain is the most common presenting complaint to our podiatrists at all our clinics. First step heel pain is a common symptom of a specific subset of heel pain which involves an overload of a structure known as the plantar fascia or plantar aponeurosis.
There are many different causes of heel pain. Take the free online heel pain test to get your results in under 60 seconds.
Plantar fasciopathy (also known as plantar fasciitis or plantar fasciosis) occurs when there is too much load or stress on the plantar fascia taking it from it’s stretchy, elastic and happy state towards its thickened, tough and painful cousin. There are many known risk factors for developing plantar fasciopathy, including the shoes we wear, the activities we do, the amount we weigh and also our bodies overall health and well being. While an expert PridePlus Health Podiatrist can help identify your individual risk factors, and also how to manage them, today we will talk about the underlying causes of plantar fasciopathy.
What is the plantar fascia?
The plantar fascia is a stretchy, elastic like band of fibrous tissue which runs from the centre middle of the heel (medial calcaneal tubercle) via 3 separate bands to the joints at the ball of the feet (the metatarsophalangeal joints). Fascia is a fascinating (or should that be fascia-nating?? OK I’ll show myself out.) structure which has some similarities to tendons and some to muscles. The similarities are that there are contractile tissues within fascia (the bits of our muscles which create a force to move), and minimal direct blood supply much like a tendon.
Some of us have more prominent plantar fascia than others. You can feel your own fascia if you sit barefoot, cross one leg onto the other so that you can extend your big toe back. As you do this you can feel your plantar fascia if you run your thumb from the centre of your heel, towards your big toe. In some people you can even see the plantar fascia running underneath the skin.
What does the it do?
The best analogy I can give for the plantar fascia in action is to think of it as a spring. Every time we plant our foot and transfer our weight down that leg our feet accommodate the movement and apply a tensile stretch to our plantar fascia. This is like pulling a spring from both ends, and it stores some energy ready for our next move. This taught, stretched spring can then help our feet maintain efficient function (walk, skip or run) by reducing some of the load on our energy hungry muscles.
So life with a good, stretchy and efficient plantar fascia is easy, as we spring from step to step. Life without this plantar fascia is much harder, as muscles must do more to maintain our stride and balance, and if we do not have that muscle strength, or we get too tired, then the extra loading gets transferred to ligaments and joints, and more problems can start.
What can go wrong with my plantar fascia?
Our plantar fascia has an optimal load capacity, which is much easier to think of in graphical form.
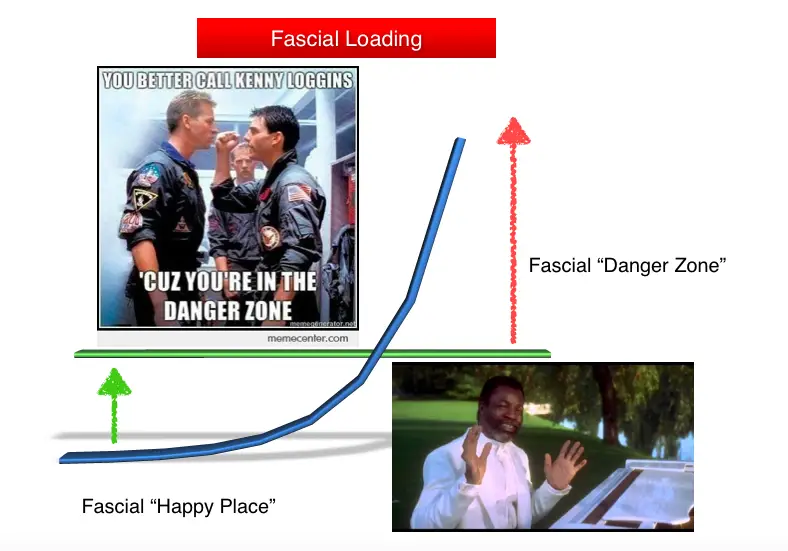
Basically we always want our plantar fascia to be loaded within our own “Happy Place” and spend as little, if any, time in the “Danger Zone” as possible.
How we load it can involve some complex engineering. Now if you’re like me and left aerospace engineering for the much more grounded and interesting career of podiatry then I’ll try to keep this straight forward. The two main loads that occur on the plantar fascia are tensile (or stretching) loads and compression. Tensile loads occur when the plantar fascia gets longer during standing when compared to non-weight bearing. Compressive loading is the squishing of the plantar fascia between our bodyweight, gravity and the ground or when we invert or evert our heel when lifting our heel off the ground (in this example to invert or evert is the tilting in or out of the heel whilst the toes are still on the ground).
How much load our plantar fascia can handle is very individual specific, and can be changed. While some factors cannot change (ie: long term steroid use, disease modifying drugs or diabetes), the ability to train it to take a higher load can be achieved although time frames and specific training protocols would need adjusting.
How can I improve my plantar fascia? Train to prevent strain.
As our plantar fascia has similarities with muscles and tendons it can be trained to increase it’s ability to do work. The training involves loading with moderate to heavy weight (that would be our bodyweight!) and doing specific exercises. We will write another post on this topic as there are lots of different methods so stay tuned for more info or if you’re suffering with plantar fasciitis, fasciopathy, fasciosis book in with a PridePlus Health Podiatrist for your personalised plan.
Where the challenge lies with training your plantar fascia is if you’re in pain because it has been working too hard, then any further exercise is going to overload it further, and make things worse, not better. This is where the tightrope act of balancing strength training to improve load capacity, and reducing current loading must be walked.
Finally, when that Monday morning alarm goes off, don’t press snooze, put on your running shoes and come visit us at PridePlus Health for an expert, individualised assessment and treatment program to overcome your heel pain.




