Are you one of the 10% of the Australian adult population of who has toenail fungus? Maybe you’re not sure but you’d really like to find out what is happening with your toenails as they look a bit different to what they used to?
Toenail fungus, also known as onychomycosis is something that us podiatrists treat every single day in our clinics across Melbourne.
We’ve seen every kind of fungal toenail and provided assessment, education and treatment to thousands of nails.
One of the most important aspects of successfully treating toenail fungus is to get an accurate and early diagnosis. If toenail fungus spreads it becomes more challenging to treat and complete resolution can impossible.
With that in mind we’ve created a simple tool for you to submit an image or video of your toenails to our podiatrists for an expert opinion. Best of all, it’s free of charge.
Want your toenails assessed by our podiatrists online? Complete the simple 4 part toenail testing tool below.
Toenail Fungus Testing Tool
Trouble loading the tool? Click to open the toenail fungal test in a new browser.
Need a podiatrist to assess or treat your toenail fungus?
Book in with our team at any of our clinics across Melbourne.
Toenail Fungus Basics
In this section we’ll talk about fungal toenails. The treatments discussed here are general advice from experienced podiatrists. They are not personal recommendations and you should discuss your own needs with your own podiatrist or medical professional.
What causes toenail fungus?
We have fungal organisms that live on our skin harmoniously with us. Known as dermatophytes these organisms can be found on nails, skin and hair and make up the skin flora.
There’s at least 3 main types of fungus that cause fungal toenails. Trichophyton rubrum, trichophyton mentagrophytes and epidermophyton floccosum.
When they spread into an infection it’s officially an infected fungal toenail.
How do you get onychomycosis or toenail fungus?
An overgrowth of dermatophytes is known as a fungal infection. When it’s on the skin of the foot it’s called tinea pedis. When it’s on the nails it’s called onychomycosis.
Fungus loves warm, enclosed and dark environments. Add in some moisture and they are in heaven.
If you think of where your toenails spend most of their time… covered up under socks and hosiery in shoes, it’s perfect for your dermatophytes to spread.
We can also “catch” a fungal toenail from outside sources. Places where fungus can live, in standing water around showers and swimming pools. We can also catch extra fungus from sharing shoes in places like bowling lanes.
Commonly toenail fungus is picked up in nail salons where strict Australian Standards on infection control are not required by law.
When we do pick up a fungal toenail from these other sources it’s often due to higher concentration of different types of fungus that our body is not used to.
Usually we keep our dermatophytes in check on our skin via our immune system and maintaining an acidic skin barrier. As we age or if we suffer from chronic diseases our immune system and skin are less effective and keeping the fungus in check and we’re more likely to get a fungal toenail.
Does stubbing your toe lead to toenail fungus?
A significant nail injury from the trauma of stubbing or dropping something on your toe can lead to a fungal toenail in a round-about way.
If you bleed under your nail and it goes black or purple there’s extra nutrients for the normal foot fungus (those dermatophytes) to grow. As it can take over 12 months to grow the bruising from your nail injury out that is a lot of time for the fungus to multiply and infect your toenails.
This post about why your toenail has gone black has you covered.
How do you prevent fungal toenails?
The first step is excellent foot hygiene and overall health. Washing, drying and avoiding moist or dry skin is a start.
Keeping your skin at a natural pH of 5.5 will also help reduce the chance of your toenails becoming fungal. Soaps are alkaline and raise the pH of skin away from normal and can lead to increased fungus growth. Washing with a soap free wash is better for prevention.
Avoiding being barefoot around areas where others walk barefoot regularly will also help. In places like communal showers or pool decks wear rubber thongs. In hotel rooms or AirBnB’s having your own slippers provides a further barrier between your feet and other fungal sources.
Next up it’s important to make sure you’re socks or shoes don’t stay wet. Change socks regularly particularly those who get sweaty feet in warm weather.
Breathable materials in shoes and socks like natural wool, bamboo or cotton will also help reduce moisture.
If you’re cutting your own toenails avoid sharing equipment with others without sterilising or disinfecting your own nippers or clippers.
And if you’re heading to a nail salon choose carefully. At a minimum you must ask that all instruments are sterilised and chairs wiped and disinfected between clients. Much better still is to head to your podiatrist for a medical pedicure where strict Australian Standards are enforced and followed.
Leaving nail polish (or shellac or SNS) on your toenails provides another occlusive layer in which toenail fungus can develop. If you must colour ensure that there are periods of time where your nails are left “nude” and allowed to breath and recover.
What does a fungal toenail look like?

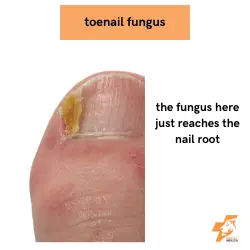
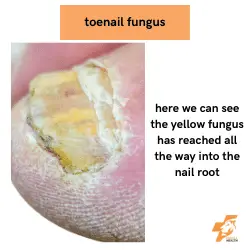
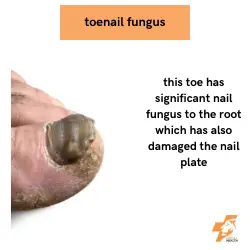
There are multiple different types of fungi that cause onychomycosis and they can present in different ways.
Sometimes you can have superficial white onychomycosis where you get chalky white spots on your toenails. This is very common after periods of nail polish use.
Other times you can have yellow-ish or brown-ish streaks within the toenail itself.
The most severe type of toenail fungus affects the nail root itself where the toenail is now discoloured, thicker and no longer smooth. There can be permanent damage to the nail root from this type of infection as well as pain as the nail can press onto healthy tissue around it.
What does toenail fungus feel like?
For many there is no feeling per se of their toenail fungus. For superficial nail infections the feeling of embarrassment is much greater than any pain.
When a toenail fungus infection deteriorates to the nail root it can be quite painful as shoes, bedsheets and other items which press onto our toenails push the deformed nail into our healthy skin.
Are fungal toenails contagious?
You can spread a fungal toenail from person to person or even toe to toe.
Toenail Fungus Treatments
To effectively treat a fungal nail infection you must have the entire fungal part of the nail either grown out or removed. You cannot “heal” the part of the nail that is currently infected. That part of a toenail does not have a direct blood supply. Side note: Imagine if it did? Wouldn’t it be awful if our toenails bled when we cut them?
For superficial toenail fungus this could mean that the entire infection can be trimmed or burred back using sterile precision equipment from your podiatrist. If this is the case the fungal toenail is 100% resolved immediately.
For most people where the toenail fungus is deeper within the toenail mechanical treatments (burring and filing) need to be combined with medicines as well.
Burring & Filing
Simple and immediate results can happen when you see your podiatrist. Utilising safe, gentle and sterile equipment your podiatrist can remove a superficial fungal nail infection immediately. If you have superficial onychomycosis then burring and filing could be your solution.
Burring and filing can also be used to increase the likelihood of success of topical medications as well as the nail plate is more open to taking on board the antifungal medicine.
Podiatrists must be careful not to thin the nail plate too much as the damage to the nail bed underneath can be quite painful.
Oral Medications
There are a couple of oral tablets that can be prescribed for toenail fungus by your GP in Australia. The most effective with the least side effects is known as terbinafine. In the past you had to have lab testing on the infected nail sampled to get oral terbinafine subsidised by the PBS.
Unfortunately growing fungus in the lab is much harder than on your foot and the testing had a high rate of false negatives. In practice this would require multiple visits to your podiatrist and GP to keep sending of more and more toenail samples until a positive result was obtained.
Luckily there is now a generic version of oral terbinafine available via prescription which is more reasonably priced.
You’ll need to get a prescription from your GP to determine if oral medication is right for you. Liver function tests are sometimes required as you’ll be taking the tablets for 3+ months in many cases.
For those who have proximal subungual onychomycosis where the infection is in the nail root oral medication is almost always necessary.
A common mistake is people thinking they need to take antibiotics for nail fungus. Bacterial infections are treated by antibiotics whereas antifungal medications are needed for nail fungus.
Topical Medications
If you pop into your chemist you’ll see lots of different options for toenail fungus treatment. Almost all of them promise to take your nails from thick and yellow to thin and clear again.
While topical medications work really well when the instructions are followed to the letter (the letter!) for superficial infections, they are not very effective for severe infections.
If the nail root is infected and the entire nail or the length of the toenail is discoloured or thick it’s not likely to get a result.
Currently our preferred topical medication available over the counter is called Loceryl. There’s plenty of risks and warnings and you should see your podiatrist before commencing treatment.
Tea tree oil is a naturally occurring antifungal which has a place treating some type of fungus on nails.
Laser or light therapies
Laser treatments for toenail fungus remains in it’s infancy. There are some early reports of successful cases although not yet outshining more effective measures.
With laser therapy a beam of light is used to heat up individual parts of the nail and nail bed to a temperature which kills the fungus but does not burn your toe.
Just like other treatments this will not “cure” your toenail and return it to looking “normal” straight away. You’ll need to have the fungal part of the toenail grow out or be cut out for that. Often topical treatments are utilised in conjunction with laser or light therapy.
Stopping the spread
For effective treatment It’s imperative to stop the spread of fungus from nail to nail or to others in your household. Ensuring your skin care is up to standard by washing with a soap free wash and drying between and around toes is the start.
Changing shoes and socks regularly and when washing using an antifungal wash additive will also help.
Thongs in your shower would be a nice touch that we’re sure your family members would appreciate as well.
If attending to your own nail care ensure you wipe the edge of your nail clippers before and after you cut your fungal toenail.
Toenail Fungus Complications
An individual toenail fungus infection, particularly if superficial is a very minor problem for most sufferers. For many, the embarrassment of having different looking toenails is the biggest driver of treatment seeking behaviours.
If left unchecked or if a onychomycosis infection spreads it can cause more significant problems.
Permanent nail deformity is likely if the nail root itself becomes infected. If you suffer with other conditions such as diabetes or poor blood circulation then a fungal toenail can lead to tissue damage, ulceration, infections and in severe (and rare) cases amputation. This is why you’re advised to see a podiatrist regularly if you have diabetes.
In other cases persistent pain can arise from a fungal toenail. The longer we have persistent pain the worse it becomes. It can lead to increase in pain sensitisation elsewhere in the body and lower the quality of day to day life.
Unchecked fungus can spread to other toenails and skin as well. A painful and serious bacterial infection can occur if the tinea pedis leads to cracks in the skin. Cellulitis or osteomyelitis are internal infections which require urgent antibiotic therapy.
What A Podiatrist Would Do
With a fungal toenail infection.
Let’s finish up with how a podiatrist would act if they hypothetically had a fungal toenail.
First, like a good podiatrist always says (and does) we’d wash daily with a soap free wash and dry between toes. This podiatrist’s personal preference is for Alphakeri wash.
Every day I would be wearing clean and dry socks and if my feet got sweaty, I’d be changing the straight away.
If the fungal infection was in the nail root I would head to my GP and arrange liver function tests to ensure I could take oral terbinafine for at last 3 months. I’d then take that medicine if I could.
However if the fungal infection was superficial (superficial onychomycosis) I would head to a fellow podiatrist who could then burr and file away all or most of the fungal reservoir on my toenail. Until my fungal toenail was completely resolved I’d be applying topical antifungals and carefully trimming my nails.
This could take 18 months if my circulation and nail growth was slow. If the infection is near the distal end of the nail or more superficial it might only take a few weeks.
Need a podiatrist to assess or treat your toenail fungus?
Book in with our team at any of our clinics across Melbourne.




