As a podiatrist with more than a dozen years experience there’s not a day goes by that I’m not asked about foot surgery. I’ll be asked for an opinion on whether Jenny’s mum should go “get her bunions done”. Or whether I think that Tony needs surgery on his “flat feet”.
Hold on. “Sir, just because I’m in my work clothes at the checkout at Woolworths doesn’t mean I can give you a full podiatry consultation. And please stop looking at the 3 packets of Tim Tams in my basket.”
Phew – ok – digression but those are real world examples of how often we podiatrists get asked about foot surgery. And not always in the professional clinical settings you’d think.
So here’s a chance for me to get it off my chest. All the information and questions about foot surgery that’s come across my path.
An important point to remember. This information is general in nature. It’s not specific to you. For that you’d need to make an appointment with say a podiatrist like the amazing team we have at PridePlus Health.
Considering foot surgery?
Be prepared with a plan by seeing our podiatry team.
So let’s get into the foot surgery information shall we?
The 8 Most Common Types of Foot and Ankle Surgery
There are many different options and sub types of foot surgery. For example there’s over 10 different surgical procedures performed for bunions. We’re going broad with these common types of foot surgery to start.
Bunion Surgery
Bunions are close to my heart, and my feet. The hardest working joint in the lower limb, the big toe joint can easily form a bunion. This is where the big toe starts to deviate towards the 2nd toe and a lump forms around the big toe joint.
As bunions are far more complex than just a lump on your foot, the various surgical procedures on them are varied. A key consideration before undergoing bunion surgery. As the big toe joint is the hardest working joint in the body, what happens after the surgery is complete? Will you be able to move the joint? Will you be able to load the joint? What activities are you expecting to do after bunion surgery?
Where us podiatrists tend to see and hear a lot of people who are disgruntled with their bunion surgery results is where these questions are not asked prior.
Because the joint is such a hard working area of our body, and there are small bones around the toe joint replacement is not really a viable option. Procedures that can give a good cosmetic result are quite straight forward (as far as a foot surgery goes). Procedures that allow for complex function and loading post surgery are much trickier, and your surgeon will need to be clear on their expectations for your foot as well.
Plantar Fasciitis Surgery
Plantar fasciitis is the most common musculoskeletal injury in the foot. It’s something that is readily and easily treated with active measures. Strengthening, footwear, orthotics and a few other modalities are all proven effective in resolving most cases of plantar fasciitis.
But there’s always outliers.
Some people who have plantar fasciitis do not respond to active measures and surgery can be required. The number of people who need this is very low, personally I have only known of one case in the last 10+ years who required surgery.
Surgical procedures for this severe, recalcitrant and chronic plantar fasciitis tend to involve lengthening the plantar fascia. For people with plantar fibromas which can present very similar to plantar fasciitis the surgical resolution is much simpler where the thick lesions are snipped away.
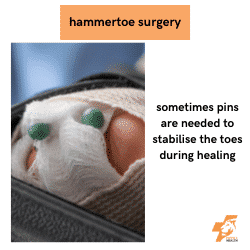
Hammertoe Surgery
Another very common surgical procedure which is performed for both cosmesis, comfort and to save limbs. Hammertoes are toes that sit up more and can rub on the top or soles of shoes. For some this means wearing fashionable shoes is impossibly painful. For others it can lead to painful corns and callus. And for those with diabetes or poor circulation they can lead to ulceration and amputation.
The surgery options for hammertoes can be as simple as tendon release procedures where local anaesthetic is used to snip a toe tendon which allow the toes to sit flat again. This does lead to weaker toes and potential balance issues however.
More complex surgical procedures that involve bone work or joint arthroplasty are needed if the hammertoe is more fixed and rigid.
Ankle Fusion Surgery
There’s no coming back from an ankle fusion. When you think how much movement and load goes through the ankle joint in all three planes (your ankle goes up, down, in, out and twists too!) a fusion to limit this movement is drastic.
But drastic injuries call for drastic measures like ankle surgery.
Chronic and complex arthritis of the rearfoot can call for an ankle fusion. As can traumatic injuries such as those that can occur if falling from a height or in motor vehicle accidents. While not yet as commonplace as knee replacement surgery, ankle joint replacements are on the rise in recent years.
Morton’s Neuroma Surgery
A Morton’s Neuroma is where the sheath around the nerve that sits between the long metatarsal bones in the foot gets too thick. This happens with chronic pressure on the nerve. Usually as a result of some instability where the metatarsals roll past and up against each other, or from tight shoes.
The surgery performed for a Morton’s Neuroma is usually a neurectomy where the thick nerve is simply cut out. As there’s unlikely to be any bone or joint involvement the recovery whilst still involved, is faster than other more complex foot surgeries. With the nerve removed there can be numbness and loss of feeling in the toes after surgery.
Ingrown Toenail Surgery
Ah, my favourite. An ingrown toenail surgery is one of the most rewarding and enjoyable procedures a podiatrist can complete.
For anyone that’s ever had an ingrown toenail, they are very, very painful. Often recurrent over many years as well.
The procedure most commonly performed for ingrown toenails is called a partial nail avulsion. Podiatrists, general practitioners, general surgeons and podiatric surgeons all perform a version of this procedure.
Flat Foot Surgery
An adult acquired flat foot, also called tibialis posterior tendon dysfunction (stage 4) is not to be confused with “having a flat foot”.
Most of us have a flatter foot shape, particularly if we are self diagnosing! Flat feet are usually very healthy and good at shock absorption and adapting to varying terrain.
Where surgery is often required is for the severe adult acquired flat foot deformity. This is where the foot loses arch height with the failure of muscles, tendons and ligaments.
It’s a big surgery, for a big injury.
Foot Surgery for Arthritis
Arthritis in the feet is as common as arthritis can get. Most of us will have arthritis changes showing up (not necessarily with any pain) through early adulthood.
If we suffer from aggressive forms of arthritis with significant pain and reduction in function there can be a number of foot surgery options to discuss. Using internal fixation to stabilise arthritic joints is common. As is “bone work” where your foot surgeon cuts away extra bone lumps that can form known as osteophytes.
Who Performs Foot Surgery In Australia
There are two surgical fields who perform complex bone and joint foot surgery in Australia. For less complex foot surgeries that only involve nails and skin podiatrists are also included.
Podiatric Surgeons
The podiatry surgery pathway is one of the most rigorous surgical training pathways in Australia. To become a podiatric surgeon you must first be a podiatrist where you complete 4 to 5 years of undergraduate training. Next, you must be accepted into the fellowship of Australian Podiatric Surgeons which requires an intense training program of more than 7 years.
Most podiatric surgeons in Australia complete large parts of their training in the USA and in Europe where there are more opportunities than in Australia. Podiatric surgery is still young in Australia and there is not the same public funding that there is for orthopaedics.
Orthopaedic Surgeons
Orthopaedic surgeons come from the medical side before moving into orthopaedics. There are many more orthopaedic surgeons than podiatric surgeons in Australia and the training is much more entrenched in the public and private health sector.
Not all orthopaedic surgeons operate on feet and you’ll find that most people report better outcomes after they see an orthopaedic surgeon who specialises in feet.
Podiatrists
OK, us podiatrists are not here for your reconstructive surgery needs. But we can provide surgical treatment for nail and skin pathologies. Ingrown toenails, warts and other superficial lesions like epidydimal cysts are all within the scope of your podiatrist.
For those podiatrist who specialise in the High Risk Foot, sharp surgical debridement is a procedure than is required for ulcer management.
While not all podiatrists are podiatric surgeons, every podiatric surgeon is a podiatrist by training. This means that there are many a great podiatric surgeon performing ingrown toenail and skin procedures. But you won’t (or shouldn’t) find a pure podiatrist conducting invasive foot surgery or playing around with a bone graft.
How To Choose A Foot Surgeon
Before you choose who is going to take a scalpel to your feet, ask yourself some important questions. Once you’ve thought about these make sure you take a list of your questions to your surgical consultations to ensure you and your surgeons expectations are consistent.
- Do I know what is wrong or why am I seeking this foot surgery?
- Have I undertaken active treatment measures with minimal risks before looking for surgery?
- What activities am I expecting to do after my foot surgery?
- 1 month after
- 3 months after
- 6 months after
- 12 months after
- How long am I going to be immobilised after my foot surgery?
- Who will help me with my daily chores? How will I commute?
- Where will I be completing my post surgical rehabilitation?
- What shoes will I be wearing after surgery? Which orthotics?
Where possible I’ll recommend clients get a couple of opinions from quality trusted surgeons. Considering the pros and cons of orthopaedic or podiatric surgery pathways. The pre surgery interview is where you’ll need to get trustworthy answers to these questions.
Now the questions aren’t to scare you. Foot surgery is not usually something to take lightly. Think of every time you take a step, hopefully there’s 10,000 of them every day. Imagine now you’ve had a surgical procedure which is going to completely change that. Every step for months will be in a different shoe or moon boot. You’ll be completing physical therapy as you get back function and range of motion. Even for weeks after surgery you could be limited to not bathing your feet and getting around with a cast on.
Respect your feet and the demands you place on them by respecting that your foot surgery isn’t complete when you wake up from the anaesthetic. For most of us, this is where the journey back to function begins.
Speed Round FAQ
Here I’ll quickly take you through the common questions thrown a podiatrists way.
What will Medicare cover for podiatric surgery?
In Australia Medicare will not cover podiatric surgery, yet. Private health insurers are now on board (some) where you can get coverage if you have podiatric surgery in your policy.
What is the long-term impact of foot fusion surgery?
Foot fusion surgery limits movement in the joints of your feet. Our feet have over 30 joints in each so that we can adjust to the different terrain on the ground, provide shock absorption, balance and efficient propulsion. If our foot joints are fused we can lose all of these superpowers and this opens ourselves up to a range of foot and lower leg complications.
But foot fusion surgery can also be very successful. If there is a true need for these procedures they can be very effective treatment of disorders like severe trauma or arthritis.
What does foot fusion surgery involve?
Foot surgery can be as quick and simple as local anaesthetic and an hour with your surgeon or podiatrist. Things that are superficial that involves nails, skin, lesions and some tendons can be over quickly and heal up in weeks.
Foot surgery that involves bone work is much more involved and the rehabilitation can be over 12 months.
Why might I need foot fusion surgery?
You might need foot surgery if you have not had success with nonsurgical treatment options or active measures. There is a wide range of reasons why ankle conditions, foot joint problems and a whole variety of conditions could benefit from foot fusion surgery.
What is minimally invasive surgery?
Minimally invasive surgery is where the surgeon uses the least amount of incisions to get the job done. For some conditions like an ingrown toenail the podiatry profession uses a partial nail avulsion to be the minimally invasive surgical option compared with a wedge resection.
For more complex bone and joint procedures minimally invasive procedures can be beneficial as healing can be much faster. A consideration is that some surgical techniques require an open field to operate in and avoiding this might compromise the amount of deep work that can be done.
What is podiatric surgery?
Podiatric surgery is performed by extensively trained podiatric surgeons in Australia. They’ll almost always operate out of a private hospital as they’re not as integrated into the public health system as orthopaedic surgeons.
Having a podiatric medicine background prior to surgery they’ll have a deep understanding of the foot and biomechanics as well as your physical and medical history.
The type of surgery performed by pod surgeons is limited to the foot and ankle but some specialise even further. A pod surgeon like Simon Smith only operates on the forefoot. Conditions such as hammertoes, hallux valgus and bunions.
What is a podiatrists role pre or post surgery?
Podiatrists are your foot and ankle experts who can help you both pre and post surgery. Pre surgery your podiatrist can actively treat, prevent, manage your needs and prepare your to be ready for your date with a surgeon.
Post surgery your podiatrist will be integral in your rehabilitation by prescribing your orthotics, adjusting your rehab program and working closely with your surgical team. Usually this will involve your surgeon, nurse and physiotherapist as well as your eager podiatrist.
How long does it take to fully recover from foot surgery?
Every foot surgery is different and your recovery time will depend a lot on you too. If you have medical conditions such as diabetes then you are at a higher risk of infection which can not only be very dangerous, but also slow your recovery rate.
Same goes for poor circulation. If you do not have enough blood flowing to your extremities then your recovery rate will be much longer.
Medicines and activity levels also play a part in how fast you recover. A very (very) broad expectation is that for superficial procedures you’ll be active again in only a couple of weeks. For complex bone and joint procedures your foot will be immobilised for at least 6 weeks with extensive rehabilitation exercises to build back function that can take over 12 months.
How long before you can walk after foot surgery?
While it depends greatly on the surgery with CAM Walkers (also known as moon boots) you might be walking within a week even if the surgery was a complex procedure.

How bad is pain after foot surgery?
Pain is so personal. It’s hard to have an answer here that covers the general advice above. Any surgery will involve some pain however you’re surgeon will be prepared with pain medications and management strategies for you.
This can include physiotherapy and orthotics via your podiatrist.
In Summary
Having foot surgery can be one of the best decisions you make. It pays to be prepared, ask questions and really understand what is going to happen to your foot, and what you and your surgeons expectations are at the end.
If you’re considering foot surgery and would like some professional and personalised advice you can book in with our podiatry team at any of our clinics across Melbourne.






