Diabetic Foot Care
Diabetic Foot Ulcers
Wounds and diabetic foot ulcers are a common occurrence for diabetics — but with the right care, they don't have to control your life.
At Pride Podiatry, we provide expert assessment, treatment, and ongoing management of diabetic foot ulcers. Early intervention is critical — the sooner you act, the better the outcome.
Book an Appointment →
What Causes Diabetic Foot Ulcers?
Diabetic ulcers develop from multiple contributing factors. Understanding the causes is the first step toward prevention and effective treatment.
Diabetic Neuropathy
Nerve damage caused by diabetes reduces sensation in the feet. This means injuries, pressure points, and irritation can go unnoticed — allowing ulcers to develop without you even realising.
Poor Circulation
Diabetes can damage blood vessels, reducing blood flow to the feet. Poor circulation slows healing and makes it harder for your body to fight infections — a dangerous combination when wounds develop.
Elevated Blood Sugar Levels
High blood glucose levels impair your body's natural healing processes and weaken the immune system, making even small wounds slower to heal and more prone to infection.
Foot Injuries & Irritation
Poorly fitting footwear, inadequate foot hygiene, improper toenail trimming, and undetected trauma from nerve damage are all external triggers that can lead to ulcer formation.
Treatment: Off-Loading
The primary treatment for diabetic foot ulcers involves removing pressure from the affected area. Off-loading is the cornerstone of healing — because without reducing pressure, even the best wound care won't get you there.
Padding & Custom Orthotics
Custom-designed to redistribute pressure away from the ulcer site and protect vulnerable areas of the foot.
CAM Walkers (Moon Boots)
Specialised walking boots that immobilise and protect the foot while allowing you to stay mobile during the healing process.
Specialised Footwear
Soft, flexible materials like neoprene reduce pressure on the foot, helping to maintain ulcer-free feet after healing.
Compression Wraps & Braces
Support healing by improving circulation and reducing swelling around the affected area.
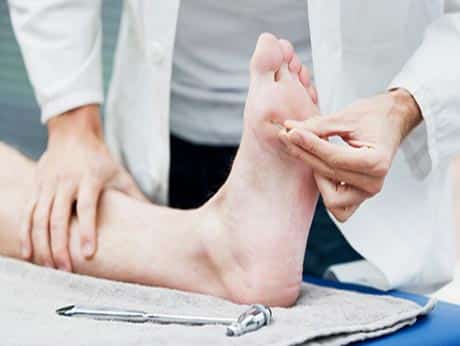
Expert Tips from Our Podiatrists
Pressure Removal is Priority
“It's what you take off, not what you put on that will heal a diabetic foot ulcer.”
Treatment focuses on eliminating pressure, removing dead tissue through debridement, and managing moisture and bacterial growth — rather than relying solely on dressings.
Footwear Matters
Appropriate shoes significantly impact healing. Soft, flexible materials like neoprene reduce pressure and help maintain ulcer-free feet. The right footwear can make or break your recovery.
Know Your Risk Level
Low risk: well-controlled diabetes with good circulation requiring annual podiatrist visits. Moderate risk: diminished circulation or pressure lesions needing regular care. High risk: severe circulation problems or loss of sensation requiring frequent neurovascular assessments.
Risk Assessment
Understanding your risk category helps determine the right level of care and monitoring for your feet.
Low Risk
Well-controlled diabetes with good circulation. Annual podiatrist visits recommended to maintain foot health and catch issues early.
Moderate Risk
Diminished circulation or pressure lesions present. Regular professional care and monitoring is essential to prevent complications.
High Risk
Severe circulation problems or loss of sensation. Frequent neurovascular assessments are critical to prevent serious complications.
Early Warning Signs
Recognising the early warning signs of diabetic foot problems can help you act fast and prevent ulcers from developing.
- !Numbness in feet
- !Itching sensations
- !Unusual temperature feelings (hot or cold)
- !Swelling or redness
- !Abnormal odors from the feet
- !Changes in skin colour or texture
- !Slow-healing cuts or blisters

Prevention Strategies
Managing diabetes effectively requires a proactive approach to foot care. Here's what you can do every day to protect your feet.
Daily Foot Washing
Wash your feet daily with soap-free cleansers. Keep the skin clean, dry between the toes, and maintain proper moisture balance to prevent cracks and infections.
Blood Sugar Monitoring
Regular blood sugar monitoring is essential. Well-controlled glucose levels improve your body's ability to heal and fight infection.
Professional Assessments
Regular podiatrist assessments catch problems early. The frequency depends on your risk level — from annual check-ups to frequent monitoring.
Circulation Management
Keep blood flowing with regular movement, avoid crossing your legs for long periods, and follow your doctor's advice on circulation support.
Proper Footwear
Wear well-fitting shoes that don't create pressure points. Avoid going barefoot and check shoes for objects before wearing them.
Toenail Care
Trim toenails carefully — straight across, not too short. If you have reduced sensation, consider professional nail care to avoid accidental injury.
Frequently Asked
Questions.
How do diabetic foot ulcers develop?
+Diabetic foot ulcers develop from a combination of nerve damage (neuropathy), poor circulation, elevated blood sugar levels, and external factors like poorly fitting footwear or undetected injuries. Nerve damage means you may not feel a wound developing, while poor circulation slows healing.
How long do diabetic foot ulcers take to heal?
+Healing time varies depending on the severity of the ulcer, your overall health, and how well blood sugar is managed. Minor ulcers may heal in weeks with proper off-loading and wound care, while more complex cases can take months. Early intervention is key to faster healing.
Can diabetic foot ulcers be prevented?
+Yes — daily foot care, proper footwear, regular blood sugar monitoring, and professional podiatrist assessments significantly reduce your risk. The earlier problems are caught, the easier they are to manage.
When should I see a podiatrist about my feet?
+If you have diabetes, you should see a podiatrist at least once a year for a diabetic foot examination — more frequently if you're at moderate or high risk. If you notice any changes in sensation, skin colour, temperature, or have a wound that isn't healing, seek assessment immediately.
What's the difference between off-loading and wound dressings?
+Off-loading removes pressure from the ulcer site, which is the most critical factor in healing. Wound dressings manage moisture and protect the wound. As our podiatrists say: 'It's what you take off, not what you put on that will heal a diabetic foot ulcer.' Both are important, but pressure removal comes first.
Don't wait. Act early.
Early intervention is the key to managing diabetic foot ulcers. Book your assessment today and take control of your foot health.
Book Now →